
In the depths of a Midwest winter, it came as no surprise that my vitamin D levels were so low – Chicago had not seen the sun in months!
And I was in good company – Research suggests that 35% of U.S. adults are vitamin D deficient, particularly those living in cooler climates.
But vitamin D is more than just the “sunshine vitamin” – It can also be absorbed through foods.
I’ll admit that I hadn’t put much thought into alternative sources of vitamin D until my doctor asked about my diet. And much to my surprise – The leading dietary source of vitamin D?
Fatty fish.
Oh, so no wonder I’m fresh out!
But the omega-3 and vitamin D recommendations made by my doctor to help supplement the lack of seafood in my diet made me wonder – Why hadn’t this been flagged sooner? Were my allergies negatively impacting my nutrition in any other ways?
So I decided to do some digging, and as it turns out, this was just the tip of the iceberg concerning the relationship between nutrition and food allergy.
Vitamin D and Allergic Disease
Vitamin D plays a significant role in immune functioning, and in turn, can impact allergic and inflammatory conditions.
Researchers have seen this phenomenon play out in surprising ways.
A study out of Australia found that peanut allergy prevalence is associated with latitude, as a function of sun exposure. The further away from the equator, the higher the rates of allergy-related hospital admissions and epinephrine prescriptions.
Another study similarly found that being born in the fall or winter months, when there is less UV exposure, is associated with higher risk for food allergy and anaphylaxis.
Any fellow Libras?
The correlation seem to go both ways.
People with food allergies may be at increased risk for nutritional deficiencies because of their dietary restrictions.
Aside from seafood, the major dietary sources of vitamin D include egg yolks and fortified foods (e.g., cow’s milk, cereal) – Most of which are top nine allergens.
This helps make sense of why vitamin D deficiency is more common among individuals with milk allergies, lactose intolerance, or those following vegan diets.
Although these associations are fascinating, vitamin D is by no means a cure all.
According to the American Academy of Allergy, Asthma, and Immunology, “It is too early to say whether vitamin D can reverse food allergies. Future research is needed to answer that question. However, research is beginning to support the idea that vitamin D can protect against food allergies and vitamin D is important for overall good health.”
Other Nutritional Risks in Allergy
Vitamin D is not alone. Food allergies and other dietary restrictions can contribute to a range of nutritional deficiencies.
Research published in Clinical Reviews in Allergy and Immunology found that children with multiple food allergies are at higher risk for inadequate nutrition intake compared to children without food allergies. And while this presents as a bigger concern for growing children, adults with food allergies may still be at risk – Especially if they are avoiding milk, wheat, or multiple foods.
This diagram from the same article is presented as a tool for providers to assess risk factors and red flags in their patients, with recommended swaps and supplements for each food being avoided.
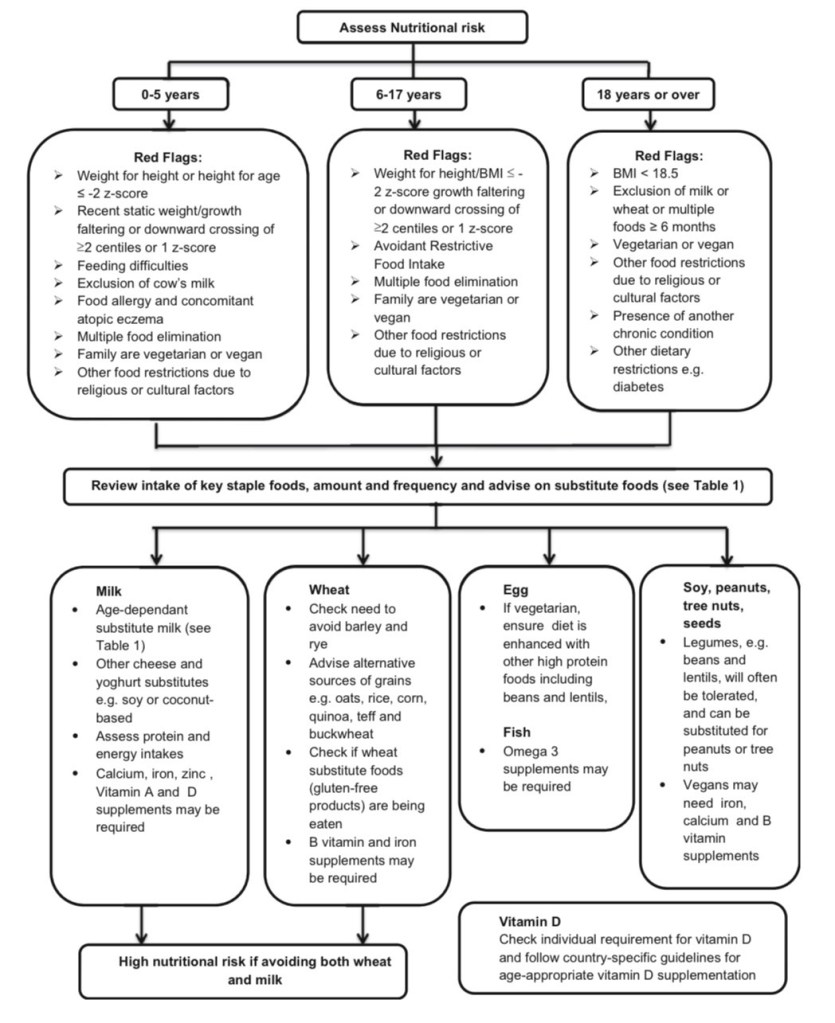
From Skypala & McKenzie, 2019
Impact on Mental Health
Hivey League – You didn’t think you were getting away without a discussion of mental heath, did you? Because the impact of vitamins and nutrients certainly does not stop at physical health.
Low levels of vitamin D are also associated with increased risk for anxiety and depression. This is thought to be one of the mechanisms behind conditions like Seasonal Affective Disorder (SAD), where decreased sun exposure can lead to a drop in serotonin production.
Omega-3 fatty acids, most commonly found in fish oils and algae, are linked to better mental health outcomes through their anti-inflammatory and mood-regulating properties. An article from Harvard Health discussed the use of Omega-3 fatty acids as an adjunct to antidepressant medication in the treatment of mood disorders.
This is actually what prompted my blood work in the first place. Incorporating functional nutrition principles into her practice, my doctor ordered a comprehensive blood panel to ensure we were supporting my mental health from all angles.
My results – which identified markers of chronic inflammation and several vitamin deficiencies – were yet another example of the complex, bidirectional relationship between my allergies and anxiety.
In All
This dynamic interplay of diet, nutrition, sun exposure, allergic disease, and mental health is exactly what I mean by food allergies are about so much more than just food.
While my new supplement routine won’t be magic pills, this functional nutrition journey has deepened my understanding of my chronic conditions and given me more power over my physical and mental health.
Plus, it has helped me get some buy in from my husband that its time to book our next beach vacation.

DISCLAIMER: The content of this post is for educational purposes only, and should not be substituted for medical or professional advice. Please consult with your doctor for more information.